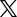-
Global Running Day

Get your legs moving on the first Wednesday of June and celebrate Global Running Day! Whether you are a regular runner or a beginner, celebrating Global Running Day can be simple and exciting. At Kentlands Foot & Ankle Center, we want to inspire and support our patients to live healthy lifestyles. Below we have curated all the ins and outs of Global Running Day.
What Is Global Running Day?
Global Running Day is a worldwide celebratory movement to encourage people of all ages to get moving. Regardless of the experience or ability, Global Running Day serves as a reminder of the power of movement and unification. No matter where you run, we are all in this together to encourage each other to keep moving, stay connected, and be healthy.
Traditions
Every year for Global Running Day, millions of people worldwide pledge to participate in some running activity by submitting their names to the Global Running Day website. Traditionally, a 5k race would be held, or folks would hit the trails. Regardless of where you decide to get moving, Global Running Day celebrates the history of running- what running means to our ancestors and what running means today.
Global Running Day in Numbers
- 59,838,621 – the number of race miles runs in the U.S. in 2020.
- 55% – the percentage of women who accounted for road race finishers in 2019.
- 518,000 – the number of Americans who finished a marathon in 2019.
- $2.46 billion – the amount spent on running shoes in 2011.
Running Self Care
At Kentlands Foot & Ankle Center, we want to remind all our patients of the importance of self-care, especially when it comes to physical activities.
- Take At Least One Rest Day a week to allow your muscles to recover and rebuild.
- Fuel Up on High-Carb, and Moderate Protein Meals 3–4 hours before a long-distance training run or event. In the 30–60 minutes leading up to a run, stick with a light, high-carb snack.
- For any run that lasts longer than 90 minutes, make sure to fuel up with a refreshing sports drink and continue to stop and take water breaks.
Visit Your Podiatrist. At least once every year, you should check in with your podiatrist. A podiatrist can examine your feet and treat any potential problems before they worsen. To schedule an appointment with our board-certified podiatrist Dr. Jon M. Sherman, at our Montgomery County office, call 301-330-5666 or visit our website for more information.
-
Pain and Injuries in the Cold Winter Months
By: Monika Twardzik-Roberts, PT
Winter seems like it’s officially here. With a seemingly mild start, the recent snow and cold temperatures make many want to stay inside and hibernate… cuddle up by the fire with a good book, watch a movie and drink hot cocoa… While these are great activities to enjoy during the winter months, making time for movement is especially important this winter as the COVID pandemic makes it easier than ever to stay sedentary for long periods of time. Finding ways to exercise and maintain healthy habits are essential to promoting a healthy well-being. The challenges of COVID have many people not feeling comfortable going to their usual public indoor exercise facilities like gyms, group fitness classes, etc. This has taken many more people outdoors for their exercise, but why do so many people have more joint pain and injuries in the winter months, and how can you decrease risk of pain/injury and find relief?
Cold weather can be especially hard on people with arthritis. The barometric pressure drops when the weather gets cold. When the pressure drops, the tissues in your joints slightly expand, which can result in increased joint pain. Synovial fluid is the shock-absorbing fluid inside the joint. The consistency is often compared to that of an egg white, allowing for unencumbered movement of your joints. In colder temperatures, the fluid thickens, resulting in stiffness or the inability for your joints to flow freely. Further, people with previous injuries may find increased pain due to nerve hypersensitivity in the cold weather.
Even those without previous pain or arthritis may find themselves at greater risk for injury. The colder temperatures impair your body’s ability to function at peak efficiency since more energy is required to maintain a normal body temperature. The limb muscles lose more heat as the body does whatever it takes to ensure your core body temperature is consistent in order to protect your vital organs. This puts the muscles, tendons, and ligaments in our legs and arms at greater risk for injury. The colder temperatures can also adversely affect the efficiency of our muscle performance as nerve impulses occur more slowly under cooler conditions. Slower reaction times due to less efficient muscle performance can lead to a higher rate of injury. Our bodies work best at an optimal temperature, so colder weather (and too hot for that matter) causes a decline in our exercise performance, especially when we are not conditioned to these temperatures.
In order to protect your body and decrease the risk of pain and/or injury as we head into the colder temperatures, warm up your muscles sufficiently, dress in layers that can be easily removed or added if you get too warm or cold, protect your head, hands, feet, and ears, and stay hydrated. Pay attention if your body starts to shiver, as this tends to be the earliest sign of potentially dangerous cold exposure. Diet can also play a part in pain due to the inflammatory nature of many foods and beverages. This is just the tip of the iceberg so to speak but can get you thinking about healthy choices for a healthy you in 2022! If you do experience an injury, old or new, don’t hesitate to contact me for personalized treatment and specialized care.
-
Bunions and How They are Treated
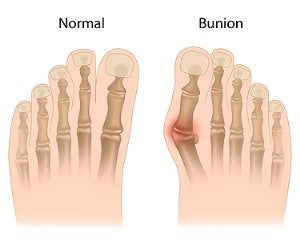 A bunion is a deformity that occurs on the joint at the base of the big toe. Though the exact cause of bunions is somewhat disputed, wearing tight fitting shoes and genetics tend to play a role in the development of exacerbation of them. Common symptoms that are usually associated with bunions include swelling, soreness, pain, and redness around the joint and bump. Bunions can become worse over time, and poorly-supportive footwear, like high heels, have been associated with worsening them. It is recommended to see a podiatrist when you notice a bunion forming even when it does not cause pain. If you have a bunion that is causing you pain, you should see one right away. A podiatrist will generally offer non-surgical options first if the bunion is not severe. These include bunions pads to relieve pressure off the bunion, pain and anti-inflammatory medication, and suggesting roomier shoes. If the pain continues or worsens and all non-surgical options have failed, surgery may be considered.
A bunion is a deformity that occurs on the joint at the base of the big toe. Though the exact cause of bunions is somewhat disputed, wearing tight fitting shoes and genetics tend to play a role in the development of exacerbation of them. Common symptoms that are usually associated with bunions include swelling, soreness, pain, and redness around the joint and bump. Bunions can become worse over time, and poorly-supportive footwear, like high heels, have been associated with worsening them. It is recommended to see a podiatrist when you notice a bunion forming even when it does not cause pain. If you have a bunion that is causing you pain, you should see one right away. A podiatrist will generally offer non-surgical options first if the bunion is not severe. These include bunions pads to relieve pressure off the bunion, pain and anti-inflammatory medication, and suggesting roomier shoes. If the pain continues or worsens and all non-surgical options have failed, surgery may be considered.
If you are suffering from bunions, contact Dr. Jon M. Sherman of Kentlands Foot & Ankle Center . Our doctor can provide the care you need to keep you pain-free and on your feet.
What is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs by the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why do Bunions Form?
- Genetics – susceptibility to bunions are often hereditary
- Stress on the feet – poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can cause bunions to form
How are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions please feel free to contact our office located in Gaithersburg, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
-
Bunions
Bunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely than men to develop bunions as well.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Initial methods to treat bunions are nonsurgical unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.
-
Tips on Exercising for Diabetics
[1].jpg) Maintaining a healthy diet and exercising can be a good way to keep your diabetes in check. However, there are some things to keep in mind and on hand if you do decide to workout. First, it is recommended to see a podiatrist to see if exercising is right for you. That being said, there are a few things that are helpful to have on hand while exercising. A blood glucose meter is a great way to check your blood sugar level before you exercise. Blood glucose tablets can help correct low blood sugar levels and ensure you are in a good state. If you do feel shaky or light-headed, it is important to relax and stop exercising. Having some snacks with you to help prevent low blood sugar is also recommended. It is important to stay hydrated while working out, especially for diabetics, because dehydration can cause high blood glucose levels. Finally, wearing a good pair of shoes is an important step in preventing foot ulcers and keeping your feet supported. Podiatrists can help recommend shoes based on your foot type or provide orthotics. Diabetes can be a difficult condition to live with; however, exercising while taking proper safety measures can be a great way to keep it in check.
Maintaining a healthy diet and exercising can be a good way to keep your diabetes in check. However, there are some things to keep in mind and on hand if you do decide to workout. First, it is recommended to see a podiatrist to see if exercising is right for you. That being said, there are a few things that are helpful to have on hand while exercising. A blood glucose meter is a great way to check your blood sugar level before you exercise. Blood glucose tablets can help correct low blood sugar levels and ensure you are in a good state. If you do feel shaky or light-headed, it is important to relax and stop exercising. Having some snacks with you to help prevent low blood sugar is also recommended. It is important to stay hydrated while working out, especially for diabetics, because dehydration can cause high blood glucose levels. Finally, wearing a good pair of shoes is an important step in preventing foot ulcers and keeping your feet supported. Podiatrists can help recommend shoes based on your foot type or provide orthotics. Diabetes can be a difficult condition to live with; however, exercising while taking proper safety measures can be a great way to keep it in check.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Jon M. Sherman of Kentlands Foot & Ankle Center . Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. Diabetes can damage blood vessels in many parts of the body, including the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels because blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Gaithersburg, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Diabetic Foot Care
-
Diabetic Foot Care
Millions of people are affected by diabetes each year. Diabetes damages blood vessels in all parts of the body, especially the feet. The legs and feet may develop slow blood flow, which causes neuropathy, or nerve damage. Once a diabetic patient develops neuropathy, it is important that the feet are well taken care of. Otherwise, the lower limbs may have to be amputated. This only happens in drastic cases, but it shows how seriously diabetic foot care should be taken.It is very important to always wash and dry the feet thoroughly, especially in between the toes, if you’re a diabetic. Secondly, examining your feet and toes for redness or sores must be done, even if you do not feel pain. You may also want to examine your feet from the bottom. Try to avoid wearing colored socks to prevent infections that may occur from the dye. Well-fitting socks are also highly recommended.
A diabetic’s physician should always monitor their blood levels to test how well blood sugars are being maintained. In addition to giving advice about everyday eating habits and foot care, a physician may prescribe medicine to help with the diabetic patient’s neuropathy. It is also advised to see a podiatrist if experiencing any feet conditions. Toenails may also need to be taken care of by a podiatrist. This prevents patients from cutting too deeply around their cuticles, which can lead to infection.
A person can take care of their feet at home by following the instructions of their physician. Using creams on one’s feet is also an effective way to heal dryness. Proceed with caution when using tools to remove calluses, as severe diabetics may not be able to feel pain on their feet. If any complications arise do not hesitate to contact a podiatrist.
On a daily basis, diabetic feet must be checked. If you are ever concerned about something, contact your health care professional. You never want to wait until a wound becomes too severe to treat. If left untreated, gangrene may develop. Gangrene is a serious infection that can lead to sepsis or amputation. It is also important for diabetics to be on the lookout for ulcers. Ulcers are sores that develop from tissue loss on the skin. They can be quite painful and require intensive treatment. Early treatment and everyday inspection are imperative to staying healthy.
-
What are Stress Fractures?
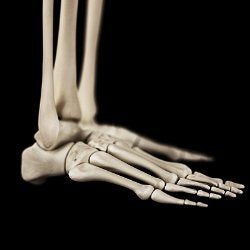 Stress fractures are small hairline fractures in the bone that most often occur from overuse. When the muscles in the body become fatigued, they become unable to handle repeated shock to the area. This shock instead transfers to the bone, which can crack. Most often, stress fractures occur in areas of the lower body like the feet and legs. The most common symptom of a stress fracture is pain in the area. If you are experiencing pain in the foot and ankle and think you may have a stress fracture, it is recommended to see a podiatrist. Rest is often the number one method in helping a stress fracture heal. Braces, pain medication, and ice may also be recommended. To prevent stress fractures, it is advised to start any new athletic activity slowly, gradually work your way up, and stop if you feel pain or have been pushing yourself with little rest.
Stress fractures are small hairline fractures in the bone that most often occur from overuse. When the muscles in the body become fatigued, they become unable to handle repeated shock to the area. This shock instead transfers to the bone, which can crack. Most often, stress fractures occur in areas of the lower body like the feet and legs. The most common symptom of a stress fracture is pain in the area. If you are experiencing pain in the foot and ankle and think you may have a stress fracture, it is recommended to see a podiatrist. Rest is often the number one method in helping a stress fracture heal. Braces, pain medication, and ice may also be recommended. To prevent stress fractures, it is advised to start any new athletic activity slowly, gradually work your way up, and stop if you feel pain or have been pushing yourself with little rest.
Activities in which too much pressure is placed on the feet can cause stress fractures. If you have any concerns about your feet contact Dr. Jon M. Sherman of Kentlands Foot & Ankle Center . Our doctor will treat your foot and ankle needs.
Dealing with Stress Fractures of the Foot and Ankle
The Stress Fractures occur on the foot and ankle when muscles in these areas weaken from too much or too little use. Then the feet and ankles lose support when walking or running from the impact of the ground. Since there is no protection the bones receive the full impact of each step. The stress on the feet causes cracks to form in the bones, thus called stress fractures.
What are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Play tennis or basketball
- Gymnastics
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures, and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity that involves in high impact will aggravate pain.
If you have any questions please feel free to contact our office located in Gaithersburg, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Stress Fractures of the Foot and Ankle
-
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person’s bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
-
Weight-Loss Surgery Found to Improve Rheumatoid Arthritis Symptoms
.jpg) A recent study published in the Arthritis Care and Research journal found that those who are obese and have rheumatoid arthritis may benefit greatly from bariatric, or weight-loss, surgery. While the study needs more research before conclusive results can be firmly established, early results note huge improvements in patients. Out of the 53 patients who have rheumatoid arthritis (RA) and undergone bariatric surgery, only six percent were found to have moderate to severe disease activity 12 months after surgery. Six years after having the surgery, 74 percent of the patients were classified as being in remission. This contrasted with the mere 24 percent achieving remission with RA medications before surgery. While these results are excellent, there are many factors that are unknown; one such factor is whether bariatric surgery is more effective in reducing RA symptoms than diet and exercise. Furthermore, bariatric surgery may potentially lead to osteoporosis. Ultimately, for those who have RA and are obese and considering bariatric surgery, there are many factors that have to be taken into account; it is best to discuss these with a doctor.
A recent study published in the Arthritis Care and Research journal found that those who are obese and have rheumatoid arthritis may benefit greatly from bariatric, or weight-loss, surgery. While the study needs more research before conclusive results can be firmly established, early results note huge improvements in patients. Out of the 53 patients who have rheumatoid arthritis (RA) and undergone bariatric surgery, only six percent were found to have moderate to severe disease activity 12 months after surgery. Six years after having the surgery, 74 percent of the patients were classified as being in remission. This contrasted with the mere 24 percent achieving remission with RA medications before surgery. While these results are excellent, there are many factors that are unknown; one such factor is whether bariatric surgery is more effective in reducing RA symptoms than diet and exercise. Furthermore, bariatric surgery may potentially lead to osteoporosis. Ultimately, for those who have RA and are obese and considering bariatric surgery, there are many factors that have to be taken into account; it is best to discuss these with a doctor.
Because RA affects more than just your joints, it is important to seek an early diagnosis from your podiatrist if you suspect that the pain in your feet may be caused by RA. For more information, contact Dr. Jon M. Sherman of Kentlands Foot & Ankle Center . Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
– Swelling & pain in the feet
– Stiffness in the feet
– Pain on the ball or sole of feet
– Joint shift and deformationDiagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in Gaithersburg, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Rheumatoid Arthritis
-
Rheumatoid Arthritis in the Feet
Although rheumatoid arthritis attacks multiple bones and joints throughout the entire body, ninety percent of people who actually develop this condition usually do so in the foot or ankle area. Those who develop this kind of arthritis in the feet usually develop symptoms around the toes and forefeet first, before anywhere else. Rheumatoid arthritis appears to have a genetic component. If it runs in the family, then you will be more likely to develop it as well.
Rheumatoid arthritis is an autoimmune disorder in which the body’s own immune system attacks the lining of the membranes surrounding the joints. This causes inflammation of the membrane lining, and the gradual destruction of the joint’s cartilage and even bone.
Some of the most common symptoms that are associated with RA include pain and swelling of the feet. Stiffness in the feet is also another common symptom that people experience. Those who have RA in the feet usually feel the pain in the ball or sole of their feet. This can get to be very painful at times. A person’s joints can even shift and become deformed after a period of time.
In order to properly diagnose RA in the feet it is usually necessary for a doctor or podiatrist to evaluate the area. Your doctor will also question you about your medical history, occupation, etc., to determine whether anything in your lifestyle may have triggered the condition. There are a number of tests that may be performed to help diagnose RA, such as a rheumatoid factor test. There is, however, no one single test that will tell you for sure if you have RA. There are different X-rays that can be taken as well to determine if a person has RA in their feet.
There is a range of treatment options for rheumatoid arthritis. Treatment of RA is usually a lifelong process that includes a variety of methods of treatment and therapy. Your doctor can prescribe special shoes that should help with arch support as well as heel support. A physical therapist can help those with this condition learn exercises which will keep their joints flexible. Surgery may be needed to correct some of the issues with the feet, such as bunions, and hammertoes. Fusion is usually the most successful surgical option for rheumatoid arthritis. However, people need to keep in mind that there are some risks associated with these surgeries.
RECENT POSTS
categories
- Uncategorized
- Featured Articles
- Foot Disorders
- Broken Ankle
- Broken Toe
- Fracture
- Foot Health
- Foot Care
- Arthritis
- Foot Pain
- Skin Cancer
- Podiatry Appointment
- Custom Orthotics
- Podiatrist
- Diabetes
- Gout
- Heart Health
- National Nutrition Month
- National Foot Health Awareness Month
- Foot Safety
- Foot and Ankle Injuries
- Falls Prevention
- Chronic Heel Pain
- Shoes
- Laser Therapy
- Quoted
- Physical Therapy
- KeryFlex
- Sweat
- Summer Foot Care
- Sports Injury
- ESWT
- Fungal Toenails
- Bunion